Gonorrhea, or “the clap,” is a sexually transmitted infection (STI). Often, gonorrhea doesn’t cause symptoms, especially in people assigned female at birth. When present, symptoms differ based on your reproductive parts. See your healthcare provider if you think you’re infected. Prompt treatment with antibiotics can prevent long-term problems.
Gonorrhea is a common sexually transmitted infection (STI) caused by a bacteria called Neisseria gonorrhoeae (N. gonorrhoeae). It’s also sometimes called “the clap” or “drip.” Gonorrhea is spread through sexual fluids, including vaginal fluid and semen. You can get gonorrhea from intercourse, anal sex, oral sex, or sharing sex toys with an infected person.
Often, gonorrhea doesn’t cause symptoms. This makes it easy to infect your partners unknowingly. Getting tested frequently — according to your healthcare provider’s recommendations — and safer sex practices can reduce your risk of infection.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Sexually active people of any age or sex can get gonorrhea and spread it to their partners. You can pass the infection on to your baby during childbirth.
You’re at greater risk of infection if you:
Gonorrhea is the second most common STI caused by bacteria – just behind chlamydia. Gonorrhea and chlamydia infections often happen together. Around 1.14 million new gonorrhea infections occur in the United States every year. About half of these infections occur in people ages 15 to 24.
Advertisement
Often, gonorrhea doesn’t cause symptoms. This is especially the case in women and people assigned female at birth (AFAB). If you do experience symptoms, they’ll likely impact you differently based on your reproductive parts.
Gonorrhea symptoms vary depending on your reproductive anatomy.
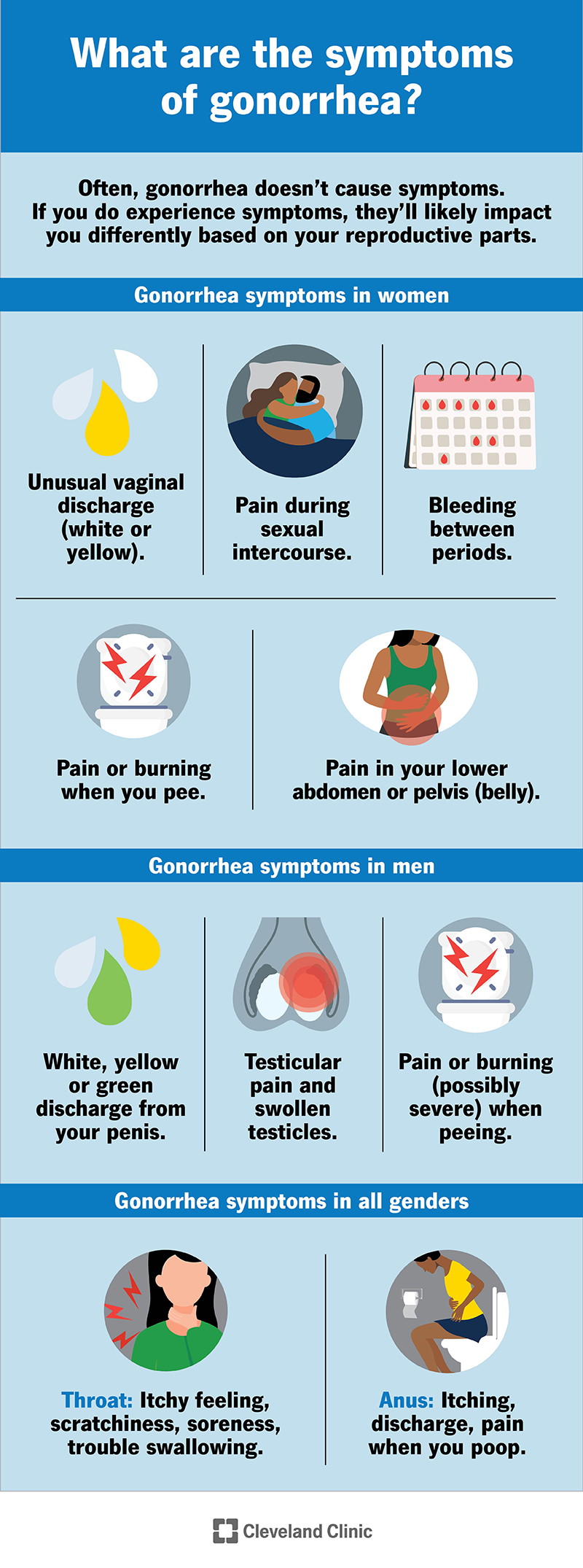
People assigned female at birth — including cisgender women, transgender men and nonbinary people with vaginas — often don’t experience symptoms. This is why it’s essential to get tested for gonorrhea if you believe you’ve been exposed.
When symptoms are present, they may include:
People assigned male at birth — including cisgender men, transgender women and nonbinary people with penises — are more likely to experience symptoms. Still, you may not notice signs of infection until several weeks after you’ve been exposed, meaning that you can unknowingly infect partners.
Symptoms may include:
People of all genders can get gonorrhea infections in the throat (through oral sex on the genitals or anus) or rectum (through anal sex). These types of infections are less common than gonorrhea affecting the genitals.
Symptoms may include:
You get an infection when the bacteria that causes gonorrhea (N. gonorrhoeae) enters your body through sexual fluids, like semen or vaginal fluid — often through unprotected sex. The bacteria can enter your body through a penis, vagina, mouth or anus. Neither you nor your partner has to ejaculate (cum) to spread the bacteria. You can also spread gonorrhea by sharing sex toys that haven’t been washed or covered with a new condom.
In people assigned female at birth, the most common site of infection is the cervix. The cervix is the opening between your vagina and your uterus.
In people assigned male at birth, infection usually starts in the urethra, the tube where urine exits your body.
Gonorrhea is contagious and spreads easily during sexual activity. Still, not all intimate acts or body fluid exchanges put you at risk for gonorrhea. You can’t get gonorrhea from:
Advertisement
You can get gonorrhea if you have sex with an infected person. This is the same, no matter your sex or gender. Vaginal intercourse, anal sex, oral sex and sharing sex toys that haven’t been cleaned or protected with a condom can all expose you to the bacteria. Close genital to genital contact without penetration can expose you, too.
Your healthcare provider will ask you questions about your symptoms and sexual history. Then, your urine or body fluid will need to be tested for the bacteria that causes gonorrhea.
During your appointment, your provider may:
Your provider will discuss which type of gonorrhea test is best in your situation and what kind of fluid sample that test requires. Your provider may also test you for chlamydia. These infections often occur together.
You’ll need antibiotics to treat gonorrhea. Your partner(s) will need treatment, too. The CDC currently recommends a shot of Ceftriaxone, with dosage based on your weight:
If you’re allergic to Cetriaxone, your healthcare provider may give you a shot of Gentamicin (240 milligrams) plus 2 grams of Azithromycin. You’ll take Azithromycin by mouth (orally).
Your provider may prescribe additional medication, like doxycycline, to clear a co-infection with chlamydia. Follow your provider’s instructions on what medications to take and when.
It’s important to consider what treatment can and can’t do. Treatment can rid your body of the bacteria. Treatment can’t:
It’s important to take preventive steps to protect yourself after treatment so that you don’t get re-infected.
Yes. Prompt treatment can cure gonorrhea. Take all medicine as your healthcare provider instructs, even if your symptoms improve and you start to feel better. Also, never take someone else’s medicine to treat your illness. Doing so makes the infection harder to treat.
Taking all antibiotics as prescribed is always important, but it’s especially important with gonorrhea. Gonorrhea is curable now, but it’s becoming more resistant to antibiotics. Some forms of gonorrhea that have developed a high level of antibiotic resistance are commonly referred to as “super gonorrhea.”
To ensure that gonorrhea remains curable, it’s more important than ever that everyone take medications as prescribed — and that everyone takes steps to prevent infection.
The only way to prevent gonorrhea is not to have sex. For many people, a more realistic goal is to reduce the risk of contracting and spreading gonorrhea. Take these steps to reduce your risk:
There’s no perfect protection for gonorrhea if you’re sexually active. For instance, condoms can tear. Still, taking extra precautions during sex can greatly reduce your risk of infection.
The CDC recommends that all people assigned female at birth who are sexually active and under 25 get tested for gonorrhea each year. Regardless of sex, you may need to get tested annually if you’re considered high risk for contracting gonorrhea. Your risk factors include your age and sexual activity. Factors like how common gonorrhea is in the area you live in are also important.
Talk to your healthcare provider about how often you should get tested based on your risk.
People who get prompt treatment and follow treatment instructions carefully can resume their normal lives. Untreated gonorrhea can cause several long-term health problems. Gonorrhea can even be life-threatening without proper care.
In people assigned female at birth, untreated gonorrhea can:
In people assigned male at birth, untreated gonorrhea can cause:
Talk to your healthcare provider. You can pass the infection on to your baby during delivery, which can cause health problems for your newborn. Babies born to birthing parents with untreated gonorrhea are at risk for complications like low birth weight and blindness.
Your provider will help you get the right testing and treatment to keep you and your baby safe.
Your healthcare provider will give you instructions about when you can resume sex. Typically, you need to wait at least a week after you and your partner(s) finish all your medications before having sex. Wait until your symptoms have gone, too.
If you are sexually active and considered high risk for gonorrhea, consider regular STI testing. Since many STIs, including gonorrhea, don’t cause symptoms, you could have an infection and pass it onto others without knowing it. Untreated gonorrhea can also cause complications that you can avoid with regular testing and prompt treatment.
If you have gonorrhea, questions you may ask include:
Begin antibiotic treatment as soon as possible. Alert your partner(s) so that they can get tested and treated, too. You may need to abstain from sex while the medicine fights the infection, but currently, antibiotics can cure gonorrhea.
A foul-smelling discharge isn’t a common symptom of gonorrhea. A smelly vaginal discharge — especially a fishy smell — may signify a vaginal infection unrelated to gonorrhea. Schedule an appointment with your provider if you notice an unusual smell and are worried about your health.
Both gonorrhea and chlamydia are highly contagious and can cause long-term damage to your health without treatment. You should avoid both infections as much as possible by practicing safer sex. Get treated immediately if you learn that you or your partner is infected.
A note from Cleveland Clinic
The best way to avoid gonorrhea is to use a condom or dental dam during any sexual activity. Safer sex is especially important with gonorrhea since it often doesn’t cause symptoms. If there’s a chance you’ve been exposed, don’t let embarrassment prevent you from scheduling a visit with your healthcare provider. Get tested immediately. Untreated gonorrhea can cause long-term damage to your health. You shouldn’t have to experience these complications, especially when a simple course of antibiotics can cure your infection.
Last reviewed on 09/02/2022.
Learn more about our editorial process.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy