Abstract
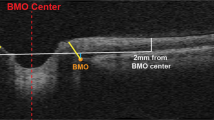
The review discusses recent foreign publications on the problem of ophthalmic changes associated with long-term effects of microgravity during space flights. The states including hyperopic shift of refraction, a change in intraocular pressure, increased intracranial pressure, alterations in the choroid and retinal tissues, and optic disk swelling have been described. These effects are caused by redistribution of blood and fluid to the upper part of the body, increased intracranial pressure, and congestion of venous blood and lymph in the upper part of the body and head. Other factors that may trigger microgravity-induced vision impairment have also been considered. Photographic illustrations of changes have been provided.
Similar content being viewed by others
References
Mader, T.H., Gibson, C.R., Pass, A.F., et al., Optic disc edema in an astronaut after repeat long-duration space flight, J. Neuro-Ophthalmol., 2013, vol. 33, no. 9, p. 249.
Alexander, D.J., Gibson, C.R., Hamilton, D.R., et al., Risk of spaceflight-induced intracranial hypertension and vision alterations, in NASA, 2012, p. 148.
Nelson, E.S., Mulugeta, L., and Myers, J.S., Microgravity-induced fluid shift and ophthalmic changes, Life, 2014, vol. 4, no. 4, p. 621.
Wotring, V.E., Space Pharmacology, New York: Springer, 2012.
Myasnikov, V.I., Stepanova S I. Risk factors for the development of neuro-psychic asthenia with an astronaut during a lengthy space flight, Vestn. Tomsk. Gos. Pedagog. Univ., 2002, vol. 31, no. 3, p. 9.
Jennings, R.T., Stepanek, J.P., Scott, L.R., and Voronkov, Y.I., Frequent premature ventricular contractions in an orbital spaceflight participant, Aviat., Space Environ. Med., 2010, vol. 81, no. 6, p. 597.
Johnston, S.L., Arenare, B.A., and Smart, K.T., Telemedicine, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 163.
Simmons, S.C., Hamilton, D.R., and McDonald, P.V., Medical imaging, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 181.
Bogomolov, V.V., Kuzmin, M.P., and Danilichev, S.N., On the intracranial hypertension in astronauts during long-term microgravity, Aviakosm. Ekol. Med., 2015, vol. 49, no. 4, p. 54.
Zhang, L.F. and Hargens, A.R., Intraocular/Intracranial pressure mismatch hypothesis for visual impairment syndrome in space, Aviat., Space Environ. Med., 2014, vol. 85, no. 1, p. 597.
Smith, S.M., Rice, B.L., Dlouhy, Y., and Zwart, S.R., Assessment of nutritional intake during space flight and space flight analogs, Procedia Food Sci., 2013, vol. 2, p. 27.
Marshall-Bowman, K., Barratt, M.R., and Gibson, C.M., Ophthalmic changes and increased intracranial pressure associated with long duration spaceflight: an emerging understanding, Acta Astronaut., 2013, vol. 87, no. 4, p. 77.
Berdahl, J.P., Fleischman, D., Allingham, R.R., and Fautsch, M., Disc swelling and space flight, Ophthalmology, 2012, vol. 119, no. 12, p. 1290.
Kramer, L.A., Sargsyan, A.E., Hasan, K.M., et al., Orbital and intracranial effects of microgravity: findings at 3-T MRimaging, Radiology, 2012, vol. 263, p. 1.
Wiener, T.C., Space obstructive syndrome: intracranial hypertension, intraocular pressure, and papilledema in space, Aviat., Space Environ. Med., 2012, vol. 83, no. 1, p. 64.
Clark, J.B. and Allen, C.S., Ophthalmologic concerns, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 535.
Partington, T. and Farmery, A., Intracranial pressure and cerebral blood flow, Anaesthes. Intensive Care Med., 2014, vol. 15, no. 4, p. 189.
Hamilton, D.R., Neurologic concerns, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 361.
Acheson, J.F., Idiopathic intracranial hypertension and visual function, Br. Med. Bull., 2006, vol. 85–86, no. 1, p. 233.
Berdahl, J.P., Yu, D.Y., and Morgan, W.M., The translaminar pressure gradient in sustained zero gravity, idiopathic intracranial hypertension, and glaucoma, Med. Hypotheses, 2012, vol. 79, no. 5, p. 719.
Marek, B., Harris, A., Kanakamedala, P., et al., Cerebrospinal fluid pressure and glaucoma: regulation of trans-lamina cribrosa pressure, Br. J. Ophthalmol., 2014, vol. 98, no. 6, p. 721.
Gilles, C., Fundamentals of Space Medicine, Amsterdam: Springer, 2006.
White, R.J. and Blomqvist, C.G., Central venous pressure and cardiac function during spaceflight, J. Appl. Physiol., 1998, vol. 85, no. 2, p. 738.
Sams, C.F. and Pierson, D.L., Cardiovascular disorders, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 317.
Hargens, A.R. and Richardson, S., Cardiovascular adaptations, fluid shifts, and countermeasures related to space flight, Respir. Physiol. Neurobiol., 2009, vol. 169, no. 10, p. 30.
Verbanck, S., Larsson, H., Linnarsson, D., et al., Pulmonary tissue volume, cardiac output, and diffusing capacity in sustained microgravity, J. Appl. Physiol., 1997, vol. 83, no. 3, p. 810.
Grigoriev, A.I., Kotovskaya, A.R., and Fomina, G.A., The human cardiovascular system during space flight, Acta Astronaut., 2011, vol. 68, no. 3, p. 1495.
Ruwanpathirana, T., Owen, A., and Reid, C.M., Review on cardiovascular risk prediction, Cardiovasc. Ther., 2015, vol. 33, no. 2, p. 62.
Kim, D.H. and Parsa, C.F., Space flight and disc edema, Ophthalmology, 2012, vol. 119, no. 11, p. 2420.
Barratt, M.R. and Pool, S.L., Human response to space flight, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 27.
Blaber, A.P., Zuj, K.A., and Goswami, N., Cerebrovascular autoregulation: lessons learned from spaceflight research, Eur. J. Appl. Physiol., 2013, vol. 113, no. 8, p. 1909.
Draeger, J., Schwartz, R., Groenhoff, S., and Stern, C., Self-tonometry under microgravity conditions, Clin. Invest., 1993, vol. 71, no. 9, p. 700.
Keith, F.M. and Mader, Th.H., Ophthalmic concerns, in Principles of Clinical Medicine for Space Flight, Barratt, M.L. and Pool, S.M, Eds., New York: Springer, 2008, p. 534.
Westfall, A.C., Ng, J.D., Samples, J.R., and Weissman, J.L., Flattening of the posterior sclera: hypotony or elevated intracranial pressure?, Am. J. Ophthalmol., 2004, vol. 138, no. 3, p. 511.
Costa, V.P. and Arcieri, E.S., Hypotony maculopathy, Acta Ophthalmol. Scand., 2007, vol. 85, no. 6, p. 586.
Keyes, L.E., Paterson, R., Boatright, D., et al., Optic nerve sheath diameter and acute mountain sickness, Wilderness Environ. Med., 2013, vol. 24, no. 2, p. 105.
Carod-Artal, F.J., High-altitude headache and acute mountain sickness, Neurologia, 2014, vol. 29, no. 9, p. 533.
Kostoglou, K., Debert, C.T., Poulin, M.J., and Mitsis, G.D., Nonstationary multivariate modeling of cerebral autoregulation during hypercapnia, Med. Eng. Phys., 2014, vol. 36, no. 5, p. 592.
James, J.T., Hypoxia, hypercarbia, and atmospheric control, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 445.
Blaha, M., Aaslid, R., Douville, C.M., et al., Cerebral blood flow and dynamic cerebral autoregulation during ethanol intoxication and hypercapnia, J. Clin. Neurosci., 2003, vol. 10, no. 2, p. 195.
Carrera, E., Lee, L.K., Giannopoulos, S., and Marshall, R.S., Cerebrovascular reactivity and cerebral autoregulation in normal subjects, J. Neurol. Sci., 2009, vol. 285, nos. 1–2, pp. 191.
Wang, D., Yee, B.J., Wong, K.K., Kim, J.W., and Dijk, D.J., Comparing the effect of hypercapnia and hypoxia on the electroencephalogram during wakefulness, Clin. Neurophysiol., 2015, vol. 126, no. 1, pp. 103–109.
Jones, J.A., Pietrzyk, R.A., and Whitson, P.A., Musculoskeletal response to space flight, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 293.
Deng, C., Wang, P., Zhang, X., and Wang, Y., Shortterm,daily exposure to cold temperature may be an efficient way to prevent muscle atrophy and bone loss in a microgravity environment, Life Sci. Space Res., 2015, vol. 5, p. 1.
Kozlovskaya, I.B., Pestov, I.D., and Egorov, A.D., The system of preventive measures in long space flights, Hum. Physiol., 2010, vol. 36, no. 7, p. 773.
Cavanagh, P.R., Genc, K.O., Gopalakrishnan, R., et al., Foot forces during typical days on the International Space Station, J. Biomech., 2010, vol. 43, no. 8, p. 2182.
Genc, K.O., Gopalakrishnan, R., Kuklis, M.M., et al., Foot forces during exercise on the International Space Station, J. Biomech., 2010, vol. 43, no. 11, p. 3020.
Loehr, J.A., Lee, S.M., English, K.L., et al., Musculoskeletal adaptations to training with the advanced resistive exercise device, Med. Sci. Sports Exercise, 2011, vol. 43, no. 1, p. 146.
Lin, Y.L., Po, H.L., Hsu, H.Y., et al., Transcranial Doppler studies on cerebral autoregulation suggest prolonged cerebral vasoconstriction in a subgroup of patients with orthostatic intolerance, Ultrasound Med. Biol., 2011, vol. 37, no. 10, p. 1554.
Talman, W.T., Dragon, D.N., and Lin, L.H., Baroreflex influences on cerebrovascular autoregulation, Auton. Neurosci., 2015, vol. 192, no. 11, p. 28.
Powers, W.J. and Zazulia, A.R., Cerebral metabolism and blood flow, in Encyclopedia of the Neurological Sciences, Elsevier, 2014, p. 683.
Mousavi, S.R., Fehlner, A., and Streitberger, K.-J., Measurement of in vivo cerebral volumetric stain induced by the Valsalva maneuver, J. Biomech., 2014, vol. 47, no. 7, p. 1652.
Rafuse, P.E., Mills, D.W., Hooper, P.L., Chang, T.S., and Wolf, R., Effects of Valsalva’s manoeuvre on intraocular pressure, Can. J. Ophthalmol., 1994, vol. 29, no. 2, p. 73.
Vieira, G.M., Oliveira, H.B., de Andrade, D.T., et al., Intraocular pressure variation during weight lifting, Arch. Opthalmol., 2006, vol. 124, no. 9, p. 1251.
Gurwood, A.S., Effects of weight lifting on intraocular pressure, Optometry, 2007, vol. 78, no. 2, p. 51.
Peters, N., Holtmannspötter, M., and Büttner, U., Valsalva- maneuver induced recurrent transient bilateral visual loss, Clin. Neurol. Neurosurg., 2011, vol. 113, no 2, p. 150.
Falcão, M., Vieira, M., Brito, P., et al., Spectraldomain optical coherence tomography of the choroid during Valsalva maneuver, Am. J. Ophthalmol., 2012, vol. 154, no. 4, p. 687.
Stamler, J., The INTERSALT Study: background, methods,findings,and implications, Am. J. Clin. Nutr., 1997, vol. 65, p. 626S.
Graudal, N., Population data on blood pressure and dietary sodium and potassium do not support public health strategy to reduce salt intake in Canadians, Can. J. Cardiol., 2016, vol. 32, no. 3, p. 283.
Hodapp, M.H., Spaceflight metabolism and nutritional support, in Principles of Clinical Medicine for Space Flight, Barratt, M.R. and Pool, S.L., Eds., New York: Springer, 2008, p. 559.
Siamwala, J.H., Rajendran, S., and Chatterjee, S., Chapter Eight–Strategies of manipulating BMP signaling in microgravity to prevent bone loss, Vitam. Horm., 2015, vol. 99, p. 249.
Stolarz-Skrzypek, K. and Staessen, J.S., Reducing salt intake for prevention of cardiovascular disease-times are changing, Adv. Chronic Kidney Dis., 2015, vol. 22, no. 2, p. 108.
Delahaye, F., Should we eat less salt? Review article, Arch. Cardiovasc. Dis., 2013, vol. 106, no. 5, p. 324.
Zwart, S.R., Gibson, C.R., Mader, T.H., et al., Vision changes after space flight are related to alterations in folate-and vitamin B-12-dependent one-carbon metabolism, J. Nutr., 2012, vol. 142, no. 3, p. 427.
Ajith, T.A., Homocysteine in ocular diseases, Clin. Chim. Acta, 2015, vol. 450, p. 316.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original Russian Text © I.A. Makarov, Y.I. Voronkov, M.G. Aslanjan, 2017, published in Fiziologiya Cheloveka, 2017, Vol. 43, No. 1, pp. 111–120.
Rights and permissions
About this article
Cite this article
Makarov, I.A., Voronkov, Y.I. & Aslanjan, M.G. Ophthalmic changes associated with long-term exposure to microgravity. Hum Physiol 43, 105–113 (2017). https://doi.org/10.1134/S0362119717010078
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0362119717010078