Abstract
Purpose
Radiation-induced oral mucositis is the most common side effect of radiotherapy in head and neck cancer; however, effective modalities for its prevention have not been established. In this study, we evaluated the effectiveness of Hangeshashinto (TJ-14), a Japanese herbal medicine, for preventing radiation-induced mucositis and elucidated its effect on inflammatory responses, including inflammatory cell chemotaxis and cyclooxygenase-2 (COX2) expression, in an animal model.
Methods
Syrian hamsters, 8–9 weeks old, were enrolled in this study. Animals were irradiated with a single 40 Gy dose to the buccal mucosa. Hamsters freely received a treatment diet mixed with 2% TJ-14 or a normal diet daily. The therapeutic effect was determined based on the visual mucositis score, body weight, and histological examination of infiltrated neutrophils and COX2 expression.
Results
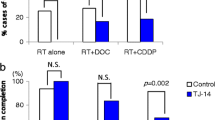
TJ-14 significantly reduced the severity of mucositis. The percentage with severe mucositis (score ≥3) was 100% in the untreated group and 16.7% in the TJ-14 group (P < 0.05). There was no difference in body weight change between the groups; however, weight gain in the untreated group tended to be suppressed compared to that in the TJ-14 group during the peak period of mucositis. In addition, TJ-14 inhibited the infiltration of neutrophils and COX2 expression in irradiated mucosa (P < 0.05).
Conclusions
TJ-14 reduced the severity of mucositis in an animal model by suppressing the inflammatory response. Because TJ-14 is inexpensive and its safety is established, it is a promising candidate for the standard treatment of radiation-induced mucositis in cancer patients.





Similar content being viewed by others
References
Calais G, Alfonsi M, Bardet E, Sire C, Germain T, Bergerot P, et al. Randomized trial of radiation therapy versus concomitant chemotherapy and radiation therapy for advanced-stage oropharynx carcinoma. J Natl Cancer Inst. 1999;91:2081–6.
Forastiere AA, Goepfert H, Maor M, Pajak TF, Weber R, Morrison W, et al. Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N Engl J Med. 2003;349:2091–8.
Trotti A, Bellm L, Epstein J, Frame D, Fuchs H, Gwede C, et al. Mucositis incidence, severity and associated outcomes in patients with head and neck cancer receiving radiotherapy with or without chemotherapy: a systematic literature review. Radiother Oncol. 2003;66:253–62.
Köstler WJ, Michael H, Catharina W, Christoph ZC. Oral mucositis complicating chemotherapy and/or radiotherapy: options for prevention and treatment. CA Cancer J Clin. 2001;51:290–351.
Russo G, Haddad R, Posner M, Machtay M. Radiation treatment breaks and ulcerative mucositis in head and neck cancer. Oncologist. 2008;13:886–98.
Lalla RV, Bowen J, Barasch A, Elting L, Epstein J, Keefe DM, et al. MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Cancer. 2014;120:1453–61.
Finch PW, Rubin JS. Keratinocyte growth factor expression and activity in cancer: implications for use in patients with solid tumors. J Natl Cancer Inst. 2006;98:812–24.
Yamashita T, Araki K, Tomifuji M, Kamide D, Tanaka Y, Shiotani A. A traditional Japanese medicine—Hangeshashinto (TJ-14)—alleviates chemoradiation-induced mucositis and improves rates of treatment completion. Support Care Cancer. 2015;23:29–35.
Kono T, Satomi M, Chisato N, Ebisawa Y, Suno M, Asama T, et al. Topical application of Hangeshashinto (TJ-14) in the treatment of chemotherapy-induced oral mucositis. World J Oncol. 2010;1:232–5.
Sonis ST, Tracey C, Shklar G, Jenson J, Florine D. An animal model for mucositis induced by cancer chemotherapy. Oral Surg Oral Med Oral Path. 1990;69:437–43.
Murphy C, Fey E, Watkins B, Wong V, Rothstein D, Sonis S. Efficacy of superoxide dismutase mimetic M40403 in attenuating radiation-induced oral mucositis in hamsters. Clin Cancer Res. 2008;14:4292–7.
Pico JL, Avila-Garavito A, Naccache P. Mucositis: its occurrence, consequences, and treatment in the oncology setting. Oncologist. 1998;3:446–51.
Sonis ST. Pathobiology of oral mucositis. Nat Rev Cancer. 2004;4:277–84.
Brock GT, McNish WR, Peters-Golden M. Arachidonic acid is preferentially metabolized by cyclooxygenase-2 to prostacyclin and prostaglandin E2. J Biol Chem. 1999;274:11660–6.
Kuehl F Jr, Egan R. Prostaglandins, arachidonic acid, and inflammation. Science. 1980;210:978–84.
Sonis ST, O’Donnell KE, Popat R, Bragdon C, Phelan S, Cocks D, et al. The relationship between mucosal cyclooxygenase-2 (COX-2) expression and experimental radiation-induced mucositis. Oral Oncol. 2004;40:170–6.
Lalla RV, Pilbeam CC, Walsh SJ, Sonis ST, Keefe DM, Peterson DE. Role of the cyclooxygenase pathway in chemotherapy-induced oral mucositis: a pilot study. Support Care Cancer. 2010;18:95.
Kaneko T, Chiba H, Horie N, Kato T, Kobayashi M, Hashimoto K, et al. Effect of Scutellariae Radix ingredients on prostaglandin E2 production and COX-2 expression by LPS-activated macrophage. In Vivo. 2009;23:577–81.
Chen YC, Shen SC, Chen LG, Lee TJF, Yang LL. Wogonin, baicalin, and baicalein inhibition of inducible nitric oxide synthase and cyclooxygenase-2 gene expressions induced by nitric oxide synthase inhibitors and lipopolysaccharide. Biochem Pharmacol. 2001;61:1417–27.
Wu P, Zhang Y, Liu Y, Wang X, Guo Z, Zhang Y, et al. Effects of glycyrrhizin on production of vascular aldosterone and corticosterone. Horm Res. 1999;51:189–92.
Hiai S, Yokoyama H, Oura H, Kawashima Y. Evaluation of corticosterone secretion-inducing activities of ginsenosides and their prosapogenins and sapogenins. Chem Pharm Bull. 1983;31:168–74.
Kase Y, Saitoh K, Ishige A, Komatsu Y. Mechanisms by which Hange-shashin-to reduces prostaglandin E2 levels. Biol Pharm Bull. 1998;21:1277–81.
Amin AH, Subbaiah TV, Abbasi KM. Berberine sulfate: antimicrobial activity, bioassay, and mode of action. Can J Microbiol. 1969;15:1067–76.
Kono T, Kaneko A, Matsumoto C, Miyagi C, Ohbuchi K, Yasuharu M, et al. Multitargeted effects of Hangeshashinto for treatment of chemotherapy-induced oral mucositis on inducible prostaglandin E2 production in human oral keratinocytes. Integr Cancer Ther. 2014;13:435–45.
Ara G, Watkins BA, Zhong H, Hawthorne TR, Karkaria CE, Sonis ST, et al. Velafermin (rhFGF-20) reduces the severity and duration of hamster cheek pouch mucositis induced by fractionated radiation. Int J Radiat Biol. 2008;84:401–12.
Hatakeyama H, Takahashi H, Oridate N, Kuramoto R, Fujiwara K, Homma K, et al. Hangeshashinto improves the completion rate of chemoradiotherapy and the nutritional status in patients with head and neck cancer. ORL J Otorhinolaryngol Relat Spec. 2015;77:100–8.
Acknowledgements
This work was supported by the National Defense Medical College Special Research Grant. We would like to thank Dr. Yoshihiro Miyagawa for technical assistance for experiments of western blot analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflict of interest.
Ethical approval
All procedures involving animals in this study were performed in accordance with the Guidelines for Proper Conduct of Animal Experiments and the US Public Health Service Policy on Human Care and Use of Laboratory Animals and were reviewed and approved by the Animal Ethical Committee of the National Defense Medical College (No. 13075).
Rights and permissions
About this article
Cite this article
Kamide, D., Yamashita, T., Araki, K. et al. Hangeshashinto (TJ-14) prevents radiation-induced mucositis by suppressing cyclooxygenase-2 expression and chemotaxis of inflammatory cells. Clin Transl Oncol 19, 1329–1336 (2017). https://doi.org/10.1007/s12094-017-1672-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-017-1672-8