Abstract
Objective
Using an animal model of preeclampsia induced by overexpression of soluble fms-like tyrosine kinase 1 (sFlt-1), we previously showed that pravastatin prevents the development of a preeclampsia phenotype. Our objective is to determine whether pravastatin treatment may be explained by its effects on apoptotic/survival pathways in the placenta.
Methods
Pregnant CD1 mice at day 8 of gestation (length of gestation 19 days) were randomly allocated to injection via tail vein with either adenovirus carrying sFlt-1 or adenovirus carrying the murine immunoglobulin G2a Fc fragment (mFc virus control group). Mice from the sFlt group were randomly assigned to receive pravastatin (5 mg/kg/d) in their drinking water from day 9 until killing (sFlt-1 ± Pravastatin) or water (sFlt-1). The mFc control received water only. Mice were killed on day 18, and the placentas were collected. Protein mitogen-activated protein kinase (MAPK) pathway substrates were assayed using Bioplex Multiplex Immunoassay (Bio- Rad, Hercules, California). Data are reported as mean + standard error of the mean or median (interquartile range) when appropriate. One-way analysis of variance followed by post hoc analysis was performed. Two-sided P value <.05 was considered statistically significant.
Results
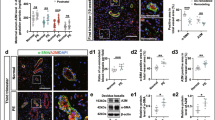
The sFlt-1 ± Pravastatin mice had significantly higher placental protein concentrations of prosurvival/ antiapoptotic factors (activating transcription factor 2, pp38, phosphorylated c-jun N-terminal kinase, and phosphorylated extracellular signal-regulated kinase) and of heat-shock protein 27 and signal transducer and activator of transcription 3, 2 factors crucial for embryonic and placental development during oxidative stress, compared to sFlt-1 mice (P <.05) and similar to the mFc control group. No differences were noted in substrates of the proapoptotic pp53 pathway.
Conclusion
Pravastatin ability to prevent preeclampsia phenotype may be mediated through pleiotropic mechanisms involving a prosurvival/ antiapoptotic MAPK pathway in the placenta. Our results further support continued research in the role for statins in the prevention of preeclampsia.
Similar content being viewed by others
References
ACOG Committee on Practice Bulletins—Obstetrics. ACOG practice bulletin. Diagnosis and management of preeclampsia and eclampsia. Number 33, January 2002. Obstet Gynecol. 2002;99(1):159–167.
Costantine MM, Cleary K; Eunice Kennedy Shriver National Institute of Child Health and Human Development Obstetric—Fetal Pharmacology Research Units Network. Pravastatin for the prevention of preeclampsia in high risk pregnant women. Obstet Gynecol. 2013;121(2 pt 1):349–353.
Lu F, Bytautiene E, Tamayo E, et al. Gender-specific effect of overexpression of SFlt-1 in pregnant mice on fetal programming of blood pressure in the offspring later in life. Am J Obstet Gynecol. 2007;197(4):418.e1-e5.
Maynard SE, Min JY, Merchan J, et al. Excess placental soluble fms-like tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J Clin Invest. 2003;111(5):649–658.
Saad AF, Kechichian T, Yin H, et al. Effects of pravastatin on angiogenic and placental hypoxic imbalance in a mouse model of preeclampsia. Reprod Sci. 2014;21(1):138–145.
Costantine MM, Tamayo E, Lu F, et al. Using pravastatin to improve the vascular reactivity in a mouse model of soluble fms-Like tyrosine kinase-1-induced preeclampsia. Obstet Gynecol. 2010;116(1):114–120.
Fox KA, Longo M, Tamayo E, et al. Effects of pravastatin on mediators of vascular function in a mouse model of soluble fms-like tyrosine kinase-1-induced preeclampsia. Am J Obstet Gynecol. 2011;205(4):366.e1–e5.
Ahmed A, Singh J, Khan Y, Seshan SV, Girardi G. A new mouse model to explore therapies for preeclampsia. PLoS One. 2010;5(10):e13663.
Kumasawa K, Ikawa M, Kidoya H, et al. Pravastatin induces placental growth factor (PGF) and ameliorates preeclampsia in a mouse model. Proc Natl Acad Sci of the U S A. 2011;108(4):1451–1455.
Singh J, Ahmed A, Girardi G. Role of complement component C1q in the onset of preeclampsia in mice. Hypertension. 2011;58(4):716–724.
Torry DS, Mukherjea D, Arroyo J, Torry RJ. Expression and function of placenta growth factor: implications for abnormal placentation. J Soc Gynecol Invest. 2003;10(4):178–188.
Levine RJ, Lam C, Qian C, et al. Circulating angiogenic factors and the risk of preeclampsia. N Engl J Med. 2004;350(7):672.
Levine RJ, Lam C, Qian C, et al. Soluble endoglin and other circulating antiangiogenic factors in preeclampsia. N Engl J Med. 2006;355(10):992–1005.
Berends AL, de Groot CJ, Sijbrands EJ, et al. Shared constitutional risks for maternal vascular-related pregnancy complications and future cardiovascular disease. Hypertension. 2008;51(4):1034–1041.
Shi GX, Jin L, Andres DA. A Rit GTPase-p38 mitogen-activated protein kinase survival pathway confers resistance to cellular stress. Mol Cell Biol. 2011;31(10):1938–1948.
Yano M, Matsumura T, Senokuchi T, et al. Statins activate peroxisome proliferator-activated receptor through extracellular signal-regulated kinase 1/2 and p38 mitogen-activated protein kinase–dependent cyclooxygenase-2 expression in macrophages. Circ Res. 2007;100(10):1442–1451.
Takenouchi Y, Kobayashi T, Matsumoto T, et al. Possible involvement of Akt activity in endothelial dysfunction in type 2 diabetic mice. J Pharmacol Sci. 2008;106(4):600–681.
Shiota M, Hikita Y, Kawamoto Y, et al. Pravastatin-induced proangiogenic effects depend upon extracellular FGF-2. J Cell Mol Med. 2012;16(9):2001–2009.
Chen JC, Huang KC, Lin WW. HMG–CoA reductase inhibitors upregulate heme oxygenase-1 expression in murine RAW264.7 macrophages via ERK, p38 MAPK and protein kinase G pathways. Cell Sign. 2006;18(1):32–39.
Hinkelmann U, Grosser N, Erdmann K, Schröder H, Immenschuh S. Simvastatin-dependent up-regulation of heme oxygenase-1 via mRNA stabilization in human endothelial cells. Eur J Pharm Sci. 2010;41(1):118–124.
Cudmore M, Ahmad S, Al-Ani B, et al. Negative regulation of soluble flt-1 and soluble endoglin release by heme oxygenase-1. Circulation. 2007;115(13):1789–1797.
Nadeau V1, Charron J. Essential role of the ERK/MAPK pathway in blood-placental barrier formation. Development. 2014;141(14):2825–2837. doi:10.1242/dev.107409.
Torry DS, Mukherjea D, Arroyo J, Torry RJ. Expression and function of placenta growth factor: implications for abnormal placentation. J Soc Gynecol Investig. 2003;10(4):178–188.
Breitwieser W, Lyons S, Flenniken AM, et al. Feedback regulation of p38 activity via ATF2 is essential for survival of embryonic liver cells. Genes Dev. 2007;21(16):2069–2082.
San Martin S, Fitzgerald JS, Weber M, et al. STAT3 and SOCS3 expression patterns during murine placenta development. Eur J Histochem. 2013;57(2):e19.
Rana S, Rajakumar A, Geahchan C, et al. Ouabain inhibits placental sFlt1 production by repressing HSP27 dependent HIF-1α pathway. FASEB J. 2014;28(10):4324–4334.
Ofori B, Rey E, Berard A. Risk of congenital anomalies in pregnant users of statin drugs. Br J Clin Pharmacol. 2007;64(4):496.
Taguchi N, Rubin ET, Hosokawa A, et al. Prenatal exposure to HMG-CoA reductase inhibitor: effects on fetal and neonatal outcomes. Reprod Toxicol. 2008;26(2):175.
Petersen EE, Mitchell AA, Carey JC, et al. Maternal exposure to statins and risk for birth defects. Am J Med Gen. 2008;146A(20):2701–2705.
Winterfeld U, Allignol A, Panchaud A, et al. Pregnancy outcome following maternal exposure to statins: a multicentre prospective study. Br J Obstet Gynaecol. 2013;120(4):463–471.
Bateman BT, Hernandez-Diaz S, Fischer MA, et al. Statins and congenital malformations: cohort study. BMJ. 2015;350:h1035.
Zarek J, Degorter MK, Lubetsky A, et al. The transfer of pravastatin in the dually perfused human placenta. Placenta. 2013;34(8):719–721.
Nanovskaya TN, Patrikeeva SL, Paul J, Costantine M, Hankins GDV, Ahmed MS. Transplacental transfer and distribution of pravastatin. Am J Obstet Gynecol. 2013;209(4):373.e1–5.
Woollett LA. Maternal cholesterol in fetal development: transport of cholesterol from the maternal to the fetal circulation. Am J Clin Nutr. 2005;82(6):1155–1161.
Ethier-Chiasson M, Duchesne A, Forest JC, et al. Influence of maternal lipid profile on placental protein expression of LDLr and SR-BI. Biochem Biophys Res Commun. 2007;359(1):8–14.
Kazmin A, Garcia-Bournissen F, Koren G. Risks of statin use during pregnancy: a systematic review. J Obstet Gynaecol Can. 2007;29(11):906–908.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Saad, A.F., Diken, Z.M., Kechichian, T.B. et al. Pravastatin Effects on Placental Prosurvival Molecular Pathways in a Mouse Model of Preeclampsia. Reprod. Sci. 23, 1593–1599 (2016). https://doi.org/10.1177/1933719116648218
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719116648218